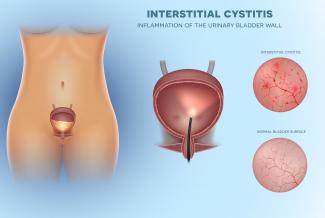
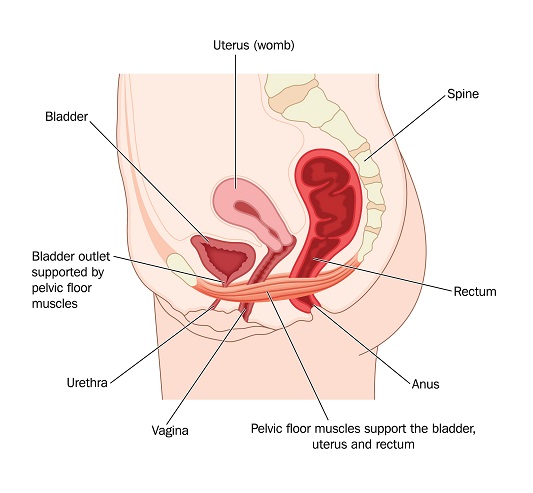
Interstitial cystitis (IC) is a long-term disorder of the bladder. The exact cause of IC is unknown. The function of the bladder is to store urine that it receives from the kidneys. You can think of the bladder as acting like a balloon made of muscle. It expands to hold large amounts of urine, and contracts to squeeze it out. The bladder expels urine into the urethra, where it comes out of the body. People who suffer from IC have bladders that are painful and stiff. Some of them develop painful ulcers or bleeding sores in their bladders. Sometimes, their bladders shrink so that they hold very little urine.

All of these things cause a person to have to urinate often. IC is more common in women than in men: About 90% of people with IC are women.[1] It occurs most often in middle-aged people, but it can occur in children or older adults.Several dietary recommendations have been shown to improve the symptoms of IC. This article will review some of the best foods to avoid (called “triggers”). Obviously, different triggers will exist for everyone, but this article will review the evidence available that would be most helpful for the average person suffering from IC.
Symptoms and Diagnosis
There are two main symptom categories for IC. The first is feeling the need to urinate often. Some people urinate up to a dozen times a day and need to get up during the night to urinate. This can be quite a burden, especially if it interferes with other aspects of life, such as being at work or being somewhere without easy access to a bathroom. The second symptom category is pain, ranging from mild to severe. The pain can get worse when the bladder fills with urine. Pain may be felt in the bladder, the urethra, the area below the belly button, the lower back, or—for women—in the area around the vagina. Men may also feel pain in their scrotum and genitals. In other words, pain can be felt anywhere around the bladder and surrounding tissues. Pain can come and go or it can be constant. It can increase during sex, and some women find that it is worse when they are having their period.[2]

Although an urgent and frequent need to urinate combined with pain are common symptoms, not everyone necessarily has both symptoms. Some people may have one symptom or the other, and they can change in intensity over time. Pain is a huge burden for those with IC, because it is directly associated with what is supposed to be a normal event that occurs multiple times daily. This can lead to additional concerns like anxiety and worrying about urination, which increases stress. It is important to identify the mental effects of IC as soon as they are happening, so that they don’t spiral and get worse. For example, stress can increase the perception of pain. So a person with IC may feel initial pain, get stressed, feel more pain, and so on. For this reason, it may also be helpful to tie any treatments of the physical body to psychological treatments.
IC is difficult to diagnose, and doctors do not agree on the best way to identify it. Most doctors will begin by examining you and asking about your symptoms. The first step in diagnosing IC is to rule out other diseases that cause similar symptoms. If that set of outcomes has been ruled out, then there are two specific lab tests that may be helpful in diagnosing IC. The first is cystoscopy. In this test, the doctor inserts a tube with lenses and light into your urethra and bladder. They may also fill the bladder with gas or liquid to test how well it can stretch. The second test is called the potassium sensitivity test. In this test, a fluid containing potassium is put into the bladder. Then you are asked to urinate. Plain water is then put into your bladder. If the potassium causes more pain or a larger need to urinate, then the test is considered positive for IC.[1] Other tests may be performed, but these are the main ones available.
Treatment Recommendations
There are several medications available for IC. The most common are pain killers, so items such as nonsteroidal anti-inflammatory drugs (ibuprofen, naproxen). Tricyclic antidepressants are also used, as they can help relax the bladder and block pain. Antihistamines can also be used, as they reduce urgency and frequency, and can sometimes relieve other symptoms.[3]

There are several lifestyle tips that can help with the intensity of IC. It’s a good idea to keep a diary of symptoms and therapies tried, because this can help to identify the best treatments over time. Gentle stretching exercises daily can be used. Learning about IC and taking an active role in treatment usually leads to better results. Drinking plenty of water (upwards of 2 L per day), even though it means urinating more, can usually be helpful. Smoking cigarettes seems to make IC worse, so try to avoid smoking, or try quitting. Finally, avoiding stressful situations is recommended because stress can make IC symptoms worse.
When it comes to clothing, there are a few factors to consider that can help with IC symptoms. Loose, comfortable clothing is recommended—basically anything that doesn’t constrict or put pressure on the crotch or surrounding areas to reduce discomfort. Cotton underwear is best and allows the skin to breathe. Avoiding coloured fabrics can be helpful, as some dyes can be irritating to the skin. Also choosing more natural laundry detergents may be a good idea. There are several ecologically friendly brands that contain less aggravating chemicals. Since chemical exposure has been noted to be one of the initiating factors for IC, reducing your chemical load can help prevent further irritation and aggravation. Since the majority of toxins and chemicals come from our self-care products and household cleaners, using more natural alternatives can be of great benefit for reducing the symptoms of IC, but also for improving overall health outcomes.
Dietary Recommendations
The following foods have been shown to have at least some association with worsening IC symptoms. As a result, it’s recommended that most IC patients choose to avoid these common trigger foods. Once again, it’s important to identify that not all people will react to the trigger foods the same way, and that an elimination diet (where these foods are eliminated for a period of time), then challenged through reintroduction is usually quite helpful. Common trigger foods to avoid in IC are:
| Alcohol |
Apples |
Aspartame |
| Avocados |
Bananas |
Cantaloupes |
| Carbonated Drinks |
Cheese |
Chicken Livers |
| Chillies/Spicy Foods |
Chocolate |
Citrus Fruits |
| Coffee |
Corned Beef |
Cranberries |
| Grapefruit |
Grapes |
Guava |
| Lemons |
Lentils |
Lima Beans |
| Limes |
Mayonnaise |
Nuts |
| Onions |
Oranges |
Peaches |
| Pickled Herring |
Pineapple |
Plums |
| Raisins |
Rye Bread |
Saccharine |
| Sour Cream |
Soy Sauce |
Strawberries |
| Yogurt |
Tomatoes |
Vinegar |
Other foods to consider eliminating: tea, carbonated beverages (cola, any and all kinds), flavour enhances of any kind (ex. peppers, chili, horseradish, vinegar, sweeteners)— including foods that commonly contain a lot of these flavour enhancers, meat (beef, pork, and lamb), and highly salty snacks like pretzels and popcorn.[4]
Lots of recipes to avoid common food triggers can be found on the Interstitial Cystitis Network website at http://www.ic-network.com/icchef/. This resource site also provides significant amounts of education to help those with IC, as well as ways to find doctors who specialize in treating IC.
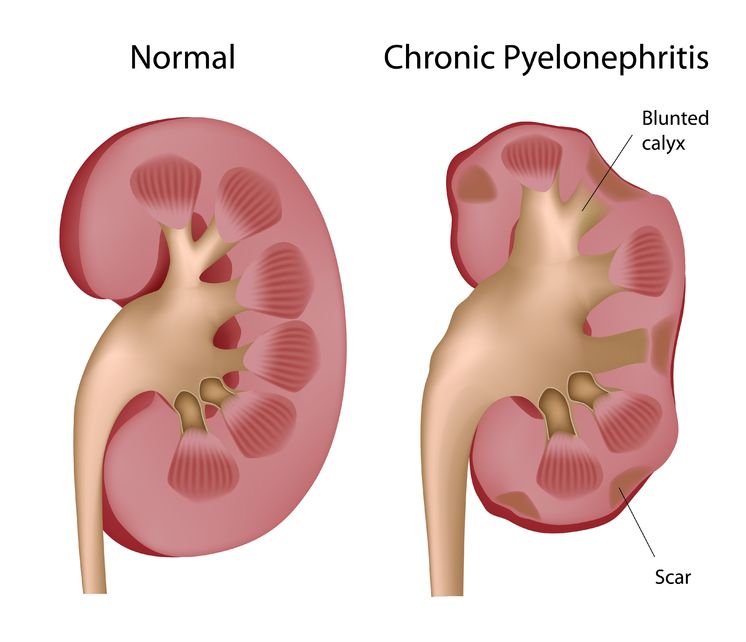
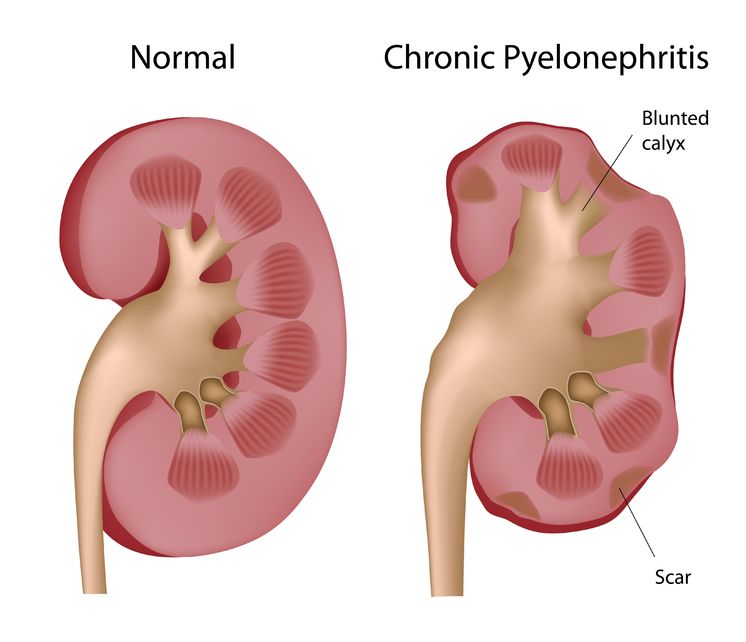 Pyelonephritis is the result of a progressive urinary tract infection, when a lower urinary infection travels upward into the upper urinary system. The lower urinary infections originate in the bladder and urethra, while the upper urinary infections involve the ureters and the kidneys. The kidneys filter the blood, so pyelonephritis can be potentially dangerous because an infection could then spread into the bloodstream.
Pyelonephritis is the result of a progressive urinary tract infection, when a lower urinary infection travels upward into the upper urinary system. The lower urinary infections originate in the bladder and urethra, while the upper urinary infections involve the ureters and the kidneys. The kidneys filter the blood, so pyelonephritis can be potentially dangerous because an infection could then spread into the bloodstream. Interstitial cystitis is a multifactorial condition and no single pathological process is present universally in patients with IC. It is thus important to determine the root causes of the individual’s symptoms, which commonly include bladder-wall dysfunction and permeability, urine acidity, and infection.
Interstitial cystitis is a multifactorial condition and no single pathological process is present universally in patients with IC. It is thus important to determine the root causes of the individual’s symptoms, which commonly include bladder-wall dysfunction and permeability, urine acidity, and infection. 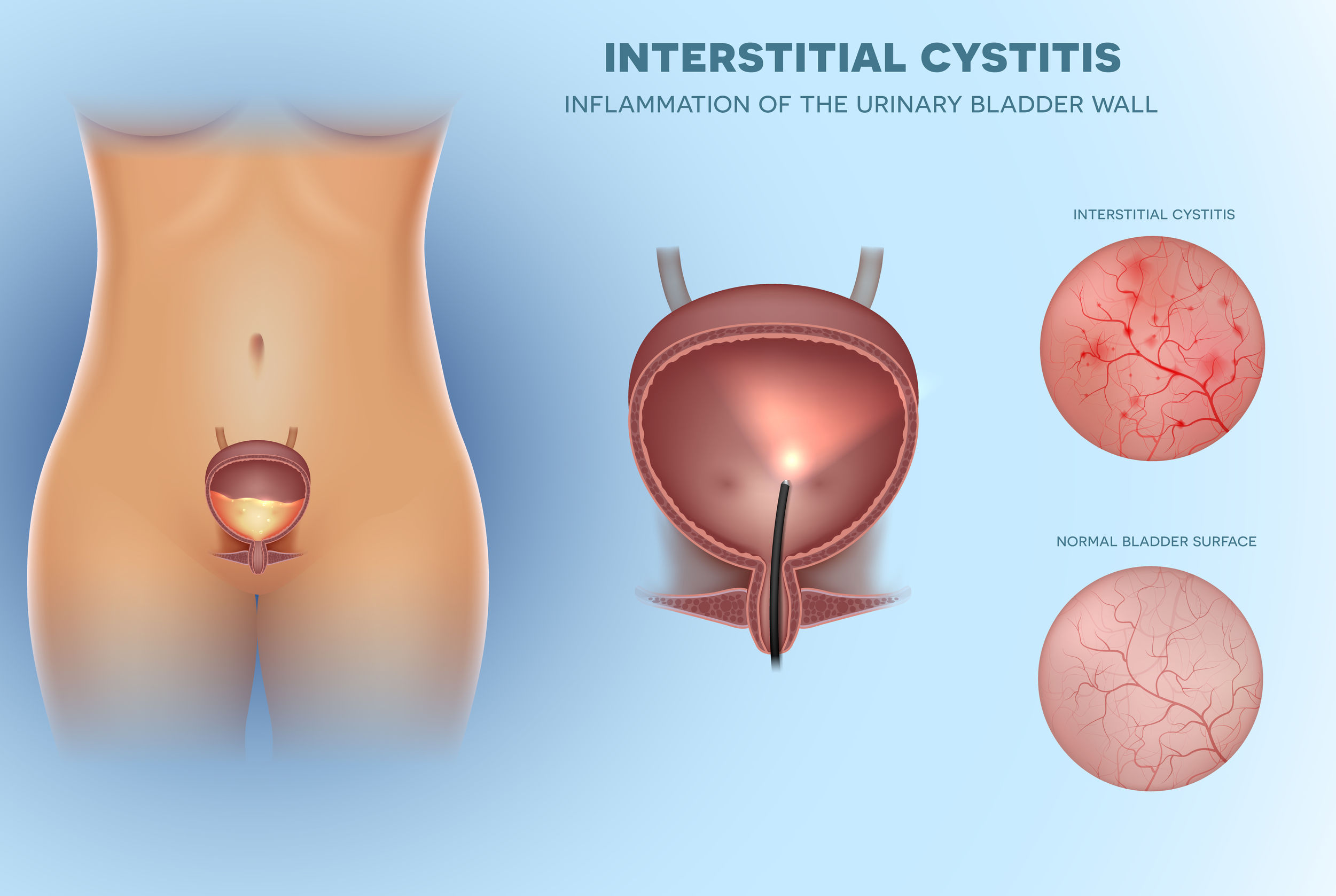 Interstitial cystitis (IC), also known as bladder pain syndrome, causes a reduced bladder capacity accompanied by symptoms of frequent, painful urination, and may or may not include blood in the urine (either seen by the naked eye or identified by urinalysis). The theory behind IC primarily emphasizes bladderwall inflammation as the root cause of symptoms. On physical examination, individuals with IC often have no physical findings, but a vague suprapubic (an area of the abdomen, just above the top of the pubic bone) tenderness may be present. The urinalysis (urine test) is often negative but may identify small/trace amounts of blood within the urine.[1]
Interstitial cystitis (IC), also known as bladder pain syndrome, causes a reduced bladder capacity accompanied by symptoms of frequent, painful urination, and may or may not include blood in the urine (either seen by the naked eye or identified by urinalysis). The theory behind IC primarily emphasizes bladderwall inflammation as the root cause of symptoms. On physical examination, individuals with IC often have no physical findings, but a vague suprapubic (an area of the abdomen, just above the top of the pubic bone) tenderness may be present. The urinalysis (urine test) is often negative but may identify small/trace amounts of blood within the urine.[1]