Related Articles
- 15 Jun 21
Medium-chain triglycerides, or MCTs, have been popularized in the context of Bulletproof™ coffee or the ketogenic diet. MCTs and the keto diet have been investigated in the management of obesity, insulin resistance, , epilepsy, neurodegenerative conditions, and others.
- 15 Jun 21
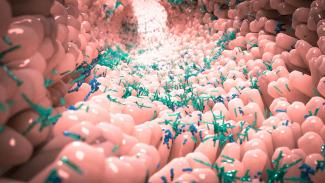
Our knowledge of connections between the human microbiome, immune system, and disease continue to evolve. Gut microbiota are influential in the health of our bodies and function to both increase immune-system function and suppress colonization of pathogens.
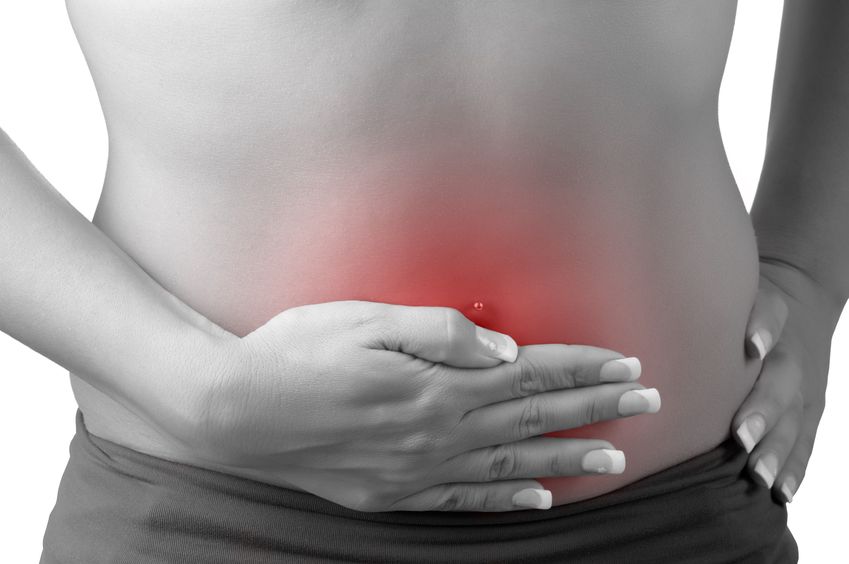
- 27 Jan 21Emerging health implications of gluten sensitivity reach far beyond the borders of the gastrointestinal tract. The gluten-sensitive spectrum includes different forms of manifestations: allergic (wheat allergy), autoimmune celiac disease (CD), dermatitis herpetiformis, gluten ataxia, and immune-mediated (nonceliac gluten sensitivity).
- 05 May 20
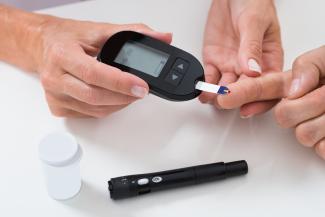
Diabetes is a common condition of the modern world, with rates of prevalence on the rise. The International Diabetes Federation estimates that in 2019, 463 million adults currently had diabetes, with a projection for this to increase to 700 million people in the next 25 years. For Canadian adults, diabetes is the number one cause of blindness, end-stage renal disease, and amputations unrelated to trauma.
- 09 Mar 20
Seasonal affective disorder (SAD) is a type of depression that is only present during the winter months. This differs from clinical depression, which has no seasonal pattern. SAD also tends to improve when the springtime occurs.
- 27 Sep 21
Naturopathic doctors talk a lot about our emotional, mental, and spiritual wellbeing since these—along with the physical—make up the four pillars of holistic health care.
- 17 Dec 19
Sadness, hopelessness and loss of interest in previously interesting activities are the hallmark of a serious, well-known mood disorder commonly referred to as depression. The Diagnostic and Statistical Manual of Mental Disorders (DSM) defines the disorder based on specific emotions that one must feel for a set amount of time.
- 16 Dec 19
In many parts of the world, attention deficit hyperactivity disorder (ADHD) is not a common diagnosis. But in North America, a large portion of the pediatric population is being screened and diagnosed with ADHD every day. While there are differences in culture and diet, could there be more that we are missing in our understanding of this developmental condition?
- 28 Jan 21Advanced glycation end-products (AGEs) are compounds that are generated under hyperglycemic conditions. They could be formed endogenously, or they could be consumed from our diet. Increased presence of AGEs in the human body is associated with diverse age-related and chronic conditions...
- 05 May 20
Coronavirus disease 2019 (COVID‑19) is a pandemic that has affected more than 200 countries all around the world, according to the World Health Organization. This disease outbreak, which started in January 2020, has shocked the world due to its uncontrollable spread and increasing death rate. Social isolation, reduced financial ability, and the lack of certainty about the future may cause symptoms of anxiety and depression in many individuals during this period. Amidst all this, many are worried about their own health status or the health of their loved ones.
- 13 Apr 20
Although it has been fraught with debate, and even disdain on occasion, the use of airbrushing of photos emanating from the marketing world of skin care and beauty tells us one thing: our society has a desire for evenness in skin appearance.
- 10 Jun 20
Depression and anxiety deplete your energy, desire, and hope. They make it difficult for you to take a step that can help you to feel better. Depression is the second most frequent medical condition seen in common medical practice around the world; it is caused by alterations of the neurotransmitters in our central nervous system.[1] It is a mood disorder that occurs differently in different individuals.
- 10 Jun 20
By now, most of us have heard the word microbiome—the collection of trillions of functional bacteria of all different species found in many places throughout our bodies, such as our skin, gut, mouth, vagina, and lungs.
- 09 Jan 20
In an ever-evolving and modernizing world, we often overlook some of the simplest things. Many cultures are based around certain foods and religious values that teach a way of life. In these cultures, practising these religious values creates a sense of community that binds the group together and further emphasizes the culture. But as families move to new cities and countries, holding on to that cultural upbringing that includes religion becomes harder and harder.
- 09 Mar 20
The viruses that cause colds and the flu can be spread easily by coughing and sneezing. While there is no way to guarantee you won’t get sick this winter, there are things you can do to reduce the severity of your sickness.
- 05 May 20
Acne (or acne vulgaris) is one of the most common skin conditions, affecting 64% of people in their 20s and 43% of people in their 30s. It affects the pilosebaceous units of the skin, which is essentially the oil gland and hair follicle. It usually affects the largest, hormone-responsive sebaceous glands such as those on the face, chest, neck and back.
- 10 Jun 20
Growing up with both parents in the teaching profession, over the years, I’ve grown accustomed to hearing commentary on “kids these days.” Lately, the conversation seems to centre around “anxious kids” or childhood anxiety. Not only do my parents see this in schools, but I hear about it all the time in my naturopathic practice from parents and even children themselves. The stats also seem to be in agreement.
- 09 Mar 20
The link between sleep and mental health has been seen and studied for decades by doctors and researchers. People who don’t get their regular 7–9 hours of sleep per night are at 10× greater risk of depression and 17× greater risk of anxiety. To go one step further, the more frequently one wakes in the night due to insomnia, the higher the chances of developing depression.[1] Before considering pharmaceutical sleeping aids, it is important that we consider all aspects of health that can be contributing to a sleep disorder.
- 08 Jul 20
With pregnancy come major changes in circulation. It’s no wonder: With an increase in body weight from the fetus and surrounding fluid, extra pressure is added onto organs and other structures like the weaker-walled veins. The body’s blood volume also increases and these changes can result in swelling, varicose veins, and hemorrhoids.
- 13 Apr 20
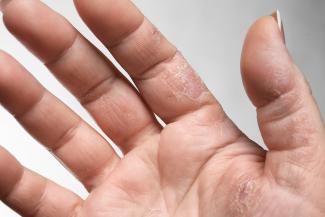
Itchy skin, dryness, redness, and cracking—uncomfortable signs of an eczema flare-up that can range from mild to having a significant impact on quality of life. Corticosteroid creams can do a fine job of targeting symptoms and inflammation associated with eczema, although below are some suggestions to get to the root cause and prevent future flare-ups.
Newsletter
Most Popular
- 03 Apr 14
- 17 Jun 13
- 17 Jun 13
- 17 Jun 13
- 01 Jul 13
- 17 Jun 13
- 17 Jun 13
- 17 Jun 13
- 01 Jul 13
- 17 Jun 13
- 17 Jun 13
- 17 Jun 13
- 01 Jul 13