Related Articles
- 15 Jun 21
Medium-chain triglycerides, or MCTs, have been popularized in the context of Bulletproof™ coffee or the ketogenic diet. MCTs and the keto diet have been investigated in the management of obesity, insulin resistance, , epilepsy, neurodegenerative conditions, and others.
- 29 Jan 21Adrenal fatigue affects individuals who suffer from a long stretch of physical, mental, environmental, or emotional stress. A “long stretch” can be defined as greater than three months. Adrenal fatigue can affect anyone, but individuals who are more likely to suffer from adrenal fatigue include single parents, individuals who are drug-dependent, those who have faced a life crisis or trauma, or those who have a stressful job circumstance.
- 27 Sep 21
Throughout the ages, humans have searched for the Fountain of Youth. Today, the search for eternal youth continues; however, we are no longer looking for a hidden fountain but instead, for lifestyle, dietary, and technological hacks we can use in attempts to delay the aging process.
- 27 Apr 22
One of the key tenants of naturopathic medicine is education. In fact, one of the guiding principles of Naturopathic Medicine is Doctor as Teacher . This principle highlights the empowering nature of naturopathic medicine. A naturopathic doctor simply provides the tools, education, and resources for each patient to work on their own healing.
- 02 Jul 14
If you are serious about athletics, or know someone who is, you already know that athletes are a slightly different breed of human. They flirt with the extreme limits of human physiology, and feed off the adrenaline it produces. Their success often hinges on the most seemingly nominal criteria: seconds, ounces, and inches.
- 17 Aug 16
- 02 Sep 15
- 17 Jun 16
 The use of complementary medicine for the treatment of cancer and its side effects has skyrocketed in recent years. Complementary therapies refer to ones that are nonpharmaceutical in nature, and that have the potential to not only enhance quality of life, but also to reduce side effects of conventional therapy.
The use of complementary medicine for the treatment of cancer and its side effects has skyrocketed in recent years. Complementary therapies refer to ones that are nonpharmaceutical in nature, and that have the potential to not only enhance quality of life, but also to reduce side effects of conventional therapy. - 17 Jun 16
- 06 Sep 16
- 13 Apr 17
- 03 Oct 16
- 21 Dec 16
- 28 Apr 22
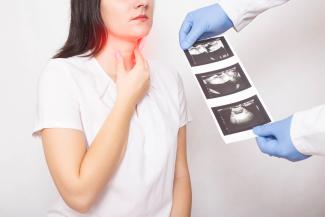
Hypothyroidism is one of the most common endocrine disorders worldwide. Hypothyroidism and subclinical hypothyroidism have a prevalence rate of 4–5% and 4–15%, respectively. The prevalence is around three to seven times higher in women than men, and its incidences proportionally increase with age.
- 15 Aug 17
- 16 Jun 21
Protocols in naturopathic practice are designed to help increase health span while taking into consideration the extent of disease, a variety of modalities or tools of applicability, and patient choice and values; however, exercise prescriptions stand out as part of a foundational approach nearly ubiquitous and necessary for almost everyone.
- 06 Nov 14
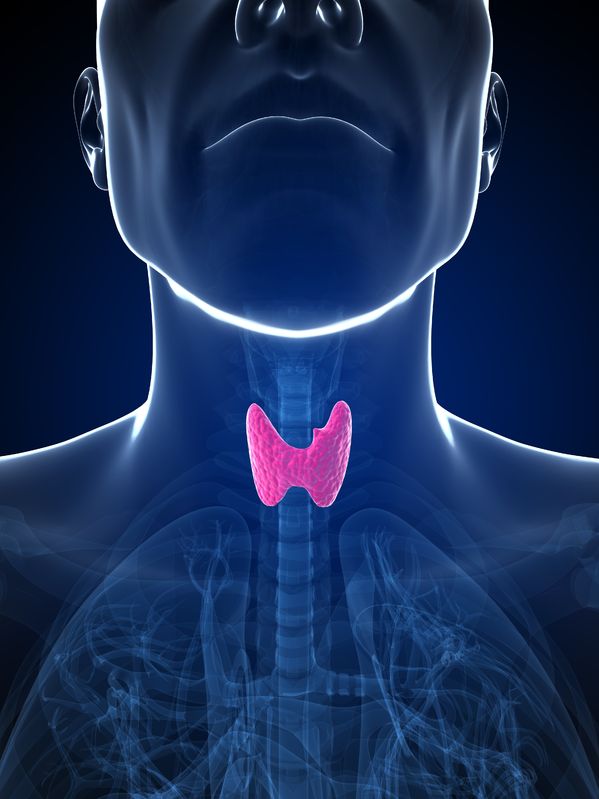
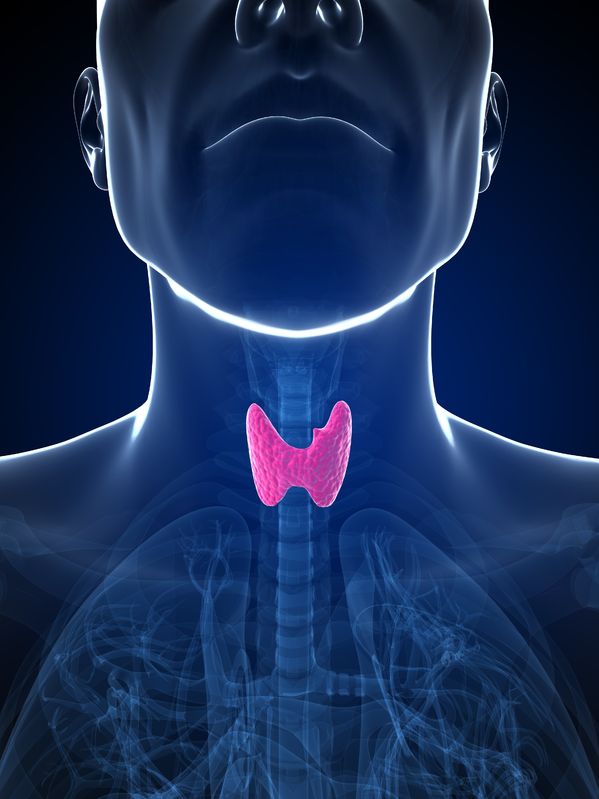 The thyroid gland is an endocrine organ responsible for metabolism in the body, regulating functions such as energy use, body temperature and heart rate. The thyroid gland first produces and secretes the hormone thyroxine (T4), generally an inactive hormone, which is then converted to its active form, triiodothyronine (T3).
The thyroid gland is an endocrine organ responsible for metabolism in the body, regulating functions such as energy use, body temperature and heart rate. The thyroid gland first produces and secretes the hormone thyroxine (T4), generally an inactive hormone, which is then converted to its active form, triiodothyronine (T3). - 03 May 17
- 01 May 21
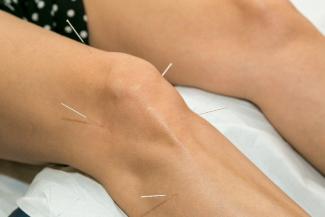
Acupuncture is a traditional therapy that has been used for thousands of years for the treatment of various ailments such as pain, fertility concerns, low energy, mood swings, and even colds and flu. It involves the insertion of very fine needles at specific points on the body to promote healing through the stimulation and circulation of “Qi.”
- 01 May 21
A holistic approach to chronic-disease prevention and treatment often includes exercise therapy as an essential modality. Exercise is generally considered a healthy activity, with few exceptions, and its application is a logical addition to any health program.
Newsletter
Most Popular
- 17 Jun 13
- 05 Jun 14
- 17 Jun 13
- 17 Jun 13
- 17 Jun 13
- 01 Jul 13
- 17 Jun 13
- 17 Jun 13
- 17 Jun 13
- 01 Jul 13
- 17 Jun 13
- 17 Jun 13
- 17 Jun 13
- 01 Jul 13